If you’ve come across this article, then you’re probably (1) a pre-health student trying to figure out the right career, (2) an applicant looking to confidently answer the question “Why PA or NP,” or (3) a curious reader who just wants to know what the difference is between these two types of providers. No matter the reason, I’m glad you’re here, and I hope you find this guide extremely helpful.
Note: My name is Phoebe, and I’m a certified PA! This article reflects my experience and observations. Obviously, I’ve been a PA student, and I’ve also had the chance to work with numerous NPs and NP students over the past several years.
There are so many healthcare jobs, and understanding the true differences between each one can be tough. The PA and NP professions are two that are compared a lot. In this article, I’ll first give you an overview of each profession. Then, I’ll go over the similarities and differences. Lastly, I’ll give a few final thoughts. Let’s get into it!
Table of Contents
Overview: What Is a Physician Associate/Assistant (PA)?
A physician associate/assistant (PA)is a medical professional with a master’s degree in PA studies who is licensed to practice medicine with physician oversight. PAs work alongside doctors to diagnose and treat patients, help deliver more efficient care, and expand access to quality healthcare. They are able to prescribe medications, perform minor procedures, and assist on major surgeries. PAs also work in a variety of specialties and subspecialties and are often responsible for the majority of direct patient care.
Note: If you’re interested in a comparison between physicians and PAs, then check out my “Doctor vs. Physician Assistant: The Pros And Cons Of Each Career Path” article
.
In order to become a PA, you must successfully complete PA school and pass the Physician Assistant National Certifying Exam (PANCE) . The last step is to apply and get approved for a state license prior to working.
. The last step is to apply and get approved for a state license prior to working.
Fun fact: Historically, PA programs awarded either a bachelor’s degree or a certificate. (That’s why you might run into some PAs without a master’s.) However, all accredited PA programs in the U.S. transitioned to a master’s degree by 2020.
Overview: What Is a Nurse Practitioner (NP)?
A nurse practitioner (NP) is a type of advanced practice registered nurse (APRN) who has completed graduate-level education and holds either a Master of Science in Nursing (MSN) or Doctor of Nursing Practice (DNP) degree. NPs are licensed to practice medicine and can diagnose and treat patients, order and interpret tests, and prescribe medications. Like PAs, they work in various specialties and subspecialties and often serve as primary care providers, particularly in underserved areas.
Note: Unlike PAs, NPs can practice independently in many states without physician oversight. (We’ll get more into this later.)
To become an NP, you must first become a registered nurse (RN) by earning a Bachelor of Science in Nursing (BSN). Then, you need to complete either an MSN or DNP program. Afterwards, you have to pass a national certification exam specific to your chosen specialty (e.g. family NP [FNP], pediatric NP [PNP], acute care NP [ACNP], etc.) through organizations like the American Nurses Credentialing Center (ANCC) or American Association of Nurse Practitioners (AANP). Finally, you must obtain state licensure to practice.
What Are the Similarities and Differences Between a Physician Assistant and Nurse Practitioner?
Similarities Between PAs & NPs
1. Roles & Responsibilities
PAs and NPs are considered advanced practice providers (APPs)—you’ll hear this term used a lot if you work in medicine. (Some other types of APPs include Certified Registered Nurse Anesthetists [CRNAs] and Certified Nurse Midwives [CNMs].) Both PAs and NPs are licensed to legally practice medicine and provide patient care. We touched on it briefly earlier, but here’s a longer list of what both a PA and NP can do:
- Conduct patient visits
- Perform physical examinations
- Order and interpret labs, tests, and imaging
- Develop treatment plans
- Prescribe medications
- Perform procedures
- First-assist in surgeries
- Provide health counseling and education
- Write referrals
In many healthcare settings, you might be seen by only a PA, only an NP, or both. The breakdown of responsibilities can vary depending on the healthcare setting, specialty, state regulations, and provider preference.
In any case, you should know that you are receiving care from professionals who have undergone extensive training. Moreover, both PAs and NPs must follow strict guidelines and regulations to ensure they are practicing within their scope and making decisions based on their patients’ best interest.
2. Patient Population & Settings
Both PAs and NPs can work in virtually any medical specialty or subspecialty. This includes primary care (e.g. family medicine, internal medicine, pediatrics, geriatrics) and specialty practice (e.g. emergency medicine, surgery, cardiology, dermatology, psychiatry, etc.). Both professions also work in diverse settings including hospitals, clinics, private practices, health centers, nursing homes, and schools.
Note: PAs tend to work in specialty care more frequently than NPs. NPs more commonly practice in primary care settings, particularly family medicine and pediatrics, where their nursing background and patient-centered approach align well with longitudinal care.
Both play crucial roles in expanding access to healthcare, particularly in underserved areas. PAs and NPs often serve as the first point of care, managing chronic conditions, performing procedures, and coordinating treatment plans.
3. Compensation & Job Outlook
PAs and NPs have similar earning potential and excellent job prospects. Median salaries are comparable, typically averaging around $130,000 annually, with variation based on specialty, location, and experience.
Moreover, both professions are among the fastest-growing occupations in healthcare, driven by an increasing population, a shortage of physicians, and greater demands for healthcare services.
Differences Between a PA & NP
1. Educational Background & Philosophy
PAs:
One of the biggest differences between PAs and NPs lies in their educational foundation and training model. Like physicians, PAs follow the medical model. PA education is modeled after that of medical school, having a strong focus on disease diagnosis and treatment.
NPs:
In contrast, NPs are trained in the nursing model, which emphasizes holistic patient care, health promotion, and disease prevention. Their education builds upon a foundation of nursing theory and practice, integrating these principles with diagnostic and prescriptive skills.
2. Length & Structure of Education
PAs:
In order to apply for PA school, you must have a bachelor’s degree in any field plus healthcare experience. PA programs typically require 500–2,000 hours of direct patient care experience (PCE) .
.
PA school itself is typically 24–28 months of intensive, in-person study. (A few PA programs are in the 31- to 33-month range.) PA programs follow a more rigid, medical school-like structure with distinct didactic and clinical phases. Due to the intensity of full-time coursework and rotations, PA students are not encouraged to work while in school.
Note: PA training is generalist by default. Rotations across a broader range of specialties (surgery, pediatrics, psychiatry, etc.) are required regardless of intended specialty.
Overall, the total time from starting undergrad to being a practicing PA is approximately 6–7 years (4 years of undergrad + 2-3 years PA school). This does not include any gap years taken to accumulate PCE hours.
NPs:
On the flip-side, NP students must first earn a BSN (4 years), work as an RN (usually 1–2 years), and then complete an MSN or DNP program. By first working as an RN, NP students are able to bring clinical nursing experience to their graduate-level education.
MSN and DNP programs usually take 2–3 years and 3–4 years, respectively, with many being part-time and/or online programs. Unlike PA students, many NP students work while attending their programs.
Note: NP training is specialist by nature. Education and training consists of coursework in a chosen specialty followed by rotations related to that specialty.
Ultimately, the total time from beginning undergrad to practicing as an NP is about 7–10 years (4 years BSN + 1–2 years RN experience + 2–4 years graduate school). Gap years aren’t relevant in this case because of the clinical experience associated with working as an RN.
Note: PA school is generally considered more competitive than NP school, given admissions GPA requirements, PCE hours, and acceptance rates (i.e. 20–31%
vs. 66%
). Additionally, there are fewer PA programs
compared to NP programs
overall. PA school also tends to be more fast-paced due to the nature of it being full-time study, whereas many NP programs offer part-time or more flexible formats that may be less intensive.
3. Ability to Practice Independently
PAs:
PAs cannot practice independently in any state. PAs are required by law to have a collaborating physician, though the level of supervision varies by state. In some states, this means the physician must be on-site; in others, the physician can be off-site.
Although PAs work quite autonomously in their day-to-day practice, they must still follow state laws and the terms of their collaboration agreement so ultimate responsibility for patient care remains shared with the physician.
Note: PA practice modernization
(formerly known as optimal team practice [OTP]) is an initiative supported by the American Academy of PAs (AAPA) that aims to give PAs more autonomy while maintaining collaborative, team-based care. In simpler terms, this effort is meant to bring PA regulations up to date and reflect how PAs actually practice today.
NPs:
Unlike PAs, NPs can practice independently in many states. As of 2025, 27 states, Washington, D.C. and two U.S. territories have adopted full practice authority (FPA) for NPs. This means that NPs in these areas can evaluate, diagnose conditions, order and interpret tests, and prescribe medications without physician oversight.
for NPs. This means that NPs in these areas can evaluate, diagnose conditions, order and interpret tests, and prescribe medications without physician oversight.
Note: Several states with FPA require a mandatory transition-to-practice period for newly licensed or less experienced NPs (i.e. typically a few thousand supervised hours) before gaining complete independence.
Other states have reduced practice (requiring a collaborative agreement with a physician for specific tasks) or restricted practice (requiring physician supervision).
4. Specialty Flexibility
PAs:
Because PAs undergo generalist training, they can easily switch specialties. PA training includes rotations in multiple specialties, and the PA certification is not specialty-specific.
This means that a PA can work in family medicine, then switch to surgery, and then move to dermatology all without additional certification or formal retraining. On-the-job training typically suffices, though some PAs choose to pursue optional residencies, fellowships, and/or specialty certifications (Certificates of Added Qualifications [CAQs] ) to demonstrate advanced expertise.
) to demonstrate advanced expertise.
NPs:
NPs are specialists from the start, which makes changing specialties harder. Much like how medical residencies work, NP education and certification are specialty-focused. An NP applicant chooses their specialty prior to applying to NP school and becomes certified in that specific area.
While NPs can work outside their specialty with appropriate training, switching specialties often requires additional certification programs, which can take one to two years and requires passing another certification exam.
5. Professional Identity & Culture
Professional rankings and perception: In U.S. News & World Report’s Best Healthcare Jobs rankings, NPs consistently rank #1, while PAs rank #2. Both professions score exceptionally well on job satisfaction, salary, and work-life balance, but NPs edge ahead in overall rankings, largely due to their independent practice authority in many states and slightly higher projected job growth.
Workforce size and advocacy power: The number of practicing providers significantly impacts each profession’s political influence and advocacy efforts. As of 2025, there are more than 461,000 NPs in the United States compared to almost 190,000 PAs
in the United States compared to almost 190,000 PAs . This ratio of around 2.4 NPs to 1 PA means that NPs have substantially greater numbers when it comes to lobbying for scope of practice expansion, influencing healthcare policy, and advocating for professional interests.
. This ratio of around 2.4 NPs to 1 PA means that NPs have substantially greater numbers when it comes to lobbying for scope of practice expansion, influencing healthcare policy, and advocating for professional interests.
Note: Larger membership numbers translate to stronger professional organizations, more political leverage, and greater visibility in healthcare policy discussions.
Professional identity: PAs identify strongly with the medical model and physician collaboration, often viewing themselves as extending the reach of physicians and working as part of a physician-led team. NPs have a distinct nursing identity and emphasize the unique perspective that nursing brings to healthcare.
Should I Become a PA or NP?
The answer to this question really depends on what you’re looking for in a career and which educational path aligns better with your background and goals. Here’s a table of the most important statistics to know regarding the PA and NP professions:
| Physician Assistant (PA) | Nurse Practitioner (NP) | |
| Median Salary | $134,000 | $129,210 |
| Average Student Loan Debt | $100,000–$200,000 | $49,000–$100,000+ |
| Projected Growth | 20% (2024-2034) (2024-2034) | 35% (2024-2034) (2024-2034) |
| Total Years of Education* | 6–7 years | 7–10 years |
| Educational Model | Medical model | Nursing model |
| Independent Practice | No (requires physician supervision) | Yes (in 27 states) |
| Specialty Flexibility | Easy to switch | Requires recertification |
Now that you have an idea of some of the stats associated with these two career paths, here are the top factors you should consider when deciding whether to become a physician assistant or nurse practitioner.
You Should Become a Physician Associate/Assistant If…
Becoming a PA may be the right fit for you if you want a faster path to practice, maximum career flexibility, and prefer the medical model of education.
- The PA route gets you practicing medicine faster. PA school is a condensed, intensive two to three years with no breaks, and you can start practicing immediately after graduation and passing the PANCE. You don’t need a nursing degree first, making it an attractive option if you’re coming from a non-nursing background. Many PA students come from diverse undergraduate majors, including biology, exercise science, psychology, or even completely unrelated fields.
- Specialty flexibility is a major advantage. As a PA, you’re not locked into one specialty for your entire career. You could theoretically work in all of the specialties without needing to return to school or obtain new certifications. This flexibility allows you to explore different areas of medicine, prevent burnout, and adapt to changing job markets or personal interests.
- You prefer the medical model of thinking. If you’re drawn to diagnosis, treatment, and the scientific approach to medicine rather than the holistic nursing framework, PA training will feel more natural. PA education closely mirrors medical school, with extensive focus on pathophysiology, differential diagnosis, and evidence-based treatment.
The main downside is that you cannot practice independently as a PA. Although changes are slowly taking place, you’ll need a collaborating physician. It’s important to mention that PAs can open their own practices. However, they still must partner with or hire a physician.
You Should Become a Nurse Practitioner If…
Becoming an NP might be best for you if you value independent practice, have a passion for nursing, and want a flexible program that will allow you to work while studying.
- Independent practice is the biggest draw. In over half of U.S. states, NPs can practice independently. As an NP, you’ll be able to see patients without physician oversight and make clinical decisions autonomously. In states with FPA, NPs can open their own practices without needing a physician on board.
- You’re passionate about the nursing perspective. If you’re drawn to the holistic, patient-centered framework that nursing brings to healthcare, then the NP path might be for you. Many NPs find deep satisfaction in combining advanced practice with nursing values.
- You prefer part-time graduate school. Unlike PA school’s intensive full-time format, many NP programs offer part-time and/or online options, allowing you to continue working as an RN while earning your advanced degree. This can reduce financial strain and lead to less student loan debt.
A key limitation to being an NP is that you can become somewhat pigeon-holed into your chosen specialty. Changing paths usually requires additional certification, exams, and one to two years of training, which can be costly and time-consuming.
Doctoral PAs & NPs
I know I’m going to get questions about this so I’ll address it briefly. As you may have noticed, the entry-level degree for PAs is a master’s, while the NP path offers both master’s and doctoral options. However, I wanted to mention that there is a doctoral option for PAs as well, and you can read more about that in my other article titled “DMSc Degrees: Everything You Need to Know About the Doctorate Degree Exclusively for Physician Assistants .”
.”
That said, remember that pursuing a doctoral degree shouldn’t be the main reason you choose a path. For many, the appeal lies in the advanced training, leadership opportunities, and deeper clinical expertise it provides—benefits that can support career advancement, teaching, or specialized practice down the line. In other words, the degree itself is less important than how it equips you with skills and experiences that align with your ultimate goals.
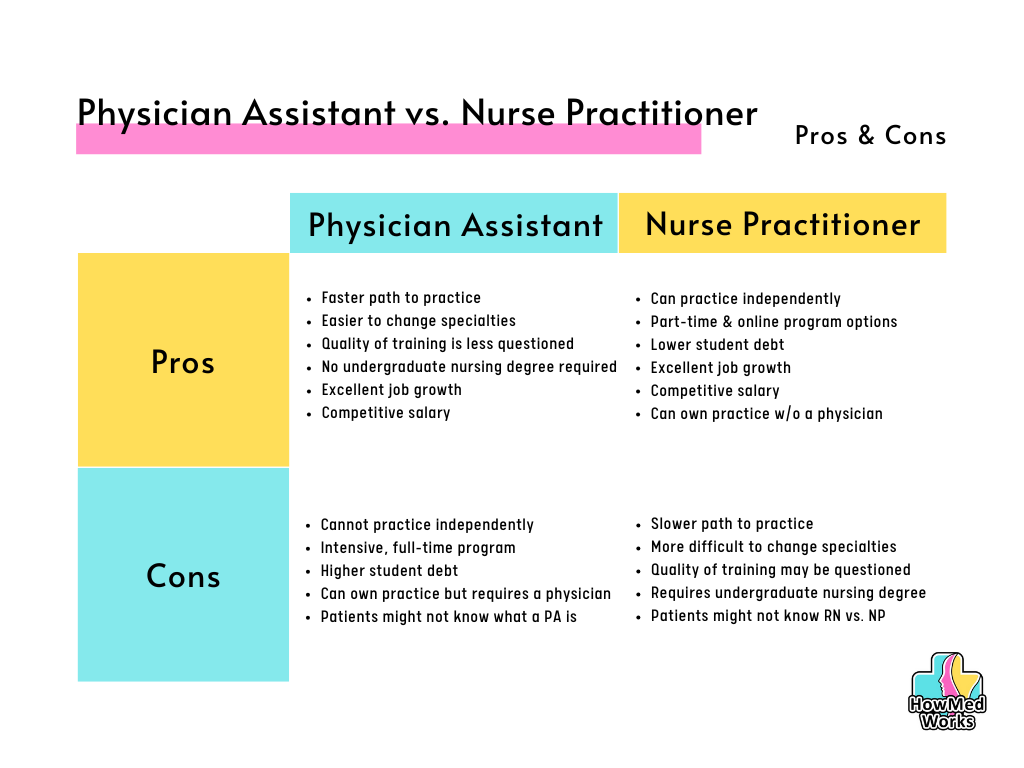
Here’s a table summarizing the main pros and cons of being a PA versus NP:
Conclusion
As you can see, both the PA and NP fields are great in their own ways, and pursuing either is highly commendable. While there is much overlap in responsibilities, there are some key differences between the PA and NP routes to take into consideration.
Consider which path aligns better with your background, values, and career goals. Both professions offer rewarding careers with excellent job prospects, competitive compensation, and the opportunity to make a real difference in patients’ lives. Hopefully now you have a thorough understanding of the two and can pick the best path for yourself!
Thanks for stopping by and, as always, stay healthy and keep learning. 😀